Roberto J. Silva Doña MD, Hector Nunez, Andrew H. Stephen
BACKGROUND
Intra-abdominal sepsis is a serious complication after anastomotic leak leading to increased mortality in patients. The use of negative pressure wound therapy (NPWT) in intra-abdominal infections has been shown to reduce morbidity and mortality compared to the combination of laparotomy, irrigation, and drainage (1). In Nicaragua, public hospitals are the main health care providers and due to budget limitations some therapeutic alternatives such as NPWT are not obtainable. These resource limited settings require providers to improvise and use the materials that are available to care for complex wounds, open abdomens, and intraabdominal infections. The following case at Hospital Escuela Antonio Lenin Fonseca (HEALF) in Managua, Nicaragua illustrates the creation and use of negative pressure wound therapy using materials readily available in a public state hospital to control intraabdominal sepsis.
PRESENTATION
A 49-year-old man was transferred to HEALF with a report of two days of leakage of intestinal fluid through his surgical wound. Three weeks prior to transfer he underwent subtotal gastrectomy and Roux- en-Y gastrojejunal anastomosis for a malignant distal gastric outlet obstruction. One week after this operation he developed a duodenal stump leak. The duodenal stump was re-sutured and a closed suction drain was placed near the stump.
Past Medical History
poorly differentiated diffuse type gastric adenocarcinoma, stage IB: T2a, N0, M0 (2)
Past Surgical History: none prior to these most recent operations
Social History: lives at home, no history of alcohol or tobacco use
PHYSICAL EXAM
On arrival to HEALF: Patient appeared unwell with decreased skin turgor and dry mucous membranes, scleral icterus. Temperature 39.6C, heart rate 110 bpm, BP 70/50 mmHg, respiratory rate 30 bpm. His initial CVP was 0mmHg. He also displayed mild abdominal distension with tenderness and green intestinal fluid output through the surgical wound.
LABS/IMAGING
WBC 16,000/mm3 (88.4% Neutrophils)
Sodium 133meq/L
Creatinine 0.5mg/dL
Lactate, bilirubin, liver enzymes and cultures were not available at the hospital’s laboratory.
Abdominal ultrasound showed fluid collections throughout the abdominal cavity.
ASSESMENT AND PLAN
Patient was diagnosed with sepsis of intra-abdominal origin causing fluid sequestration and significant intravascular fluid deficit.
HOSPITAL COURSE
Blood pressure was successfully normalized after goal oriented fluid resuscitation to a CVP of 8-12 mmHg and broad spectrum antibiotics were initialized. After the patient was stabilized he was taken to the operating room for to establish source control of intraabdominal sepsis. A 300ml purulent collection in the pelvic cavity and intense visceral adhesions were found. The intra-abdominal viscera were fused and did not allow clear anatomic planes for dissection such that the source of the leakage was not identified in this initial surgery. Abdominal lavage was carried out and closed suction drains were placed before skin closure.
In the first 24 hours postoperatively large amounts of intestinal fluid output were observed through the surgical wound and drains. The patient was taken to the OR on hospital day two and a dehiscence in the gastrojejunal anastomosis was identified. The dehiscence was managed by placement of a 32 Fr Foley catheter and its balloon was filled with 20 ml of water. The opposite end of the catheter was percutaneously exteriorized through the right flank making this a gastrostomy tube. The abdomen could not be closed due to hollow visceral distension. One commercial negative pressure wound therapy kit was available having been given by a private donation a few weeks earlier. It was placed to contain and control intraabdominal fluid and any ongoing leakage from the failed anastomosis.
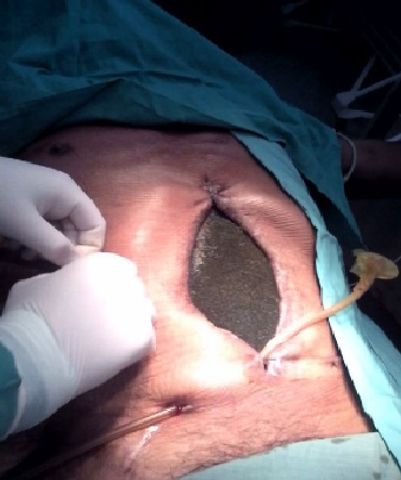
The NPWT was connected to a suction device providing 80 mmHg of negative pressure and the drainage gastrostomy was connected to a collection bag. The next day’s lab results showed a noticeable decrease in leukocytes (9,900/mm3, 77% neutrophils) and the patient no longer had fevers.
Three days later the NPWT needed replacement and no commercially designed kits for NPWT were available. An emulation with the available hospital materials was improvised. First, an extended IV bag with fenestrations was placed over the viscera(interface layer) then sterile cotton gauze pads were placed above this but within the wound. For suction tubing, two 32 French Foley catheters were placed in the gauze pads and exteriorized percutaneously. Finally, a self-adherent sterile polyethylene film was placed in a two layer fashion. The first layer covered the surgical wound and the second layer covered the entire abdomen, thus creating a complete seal.
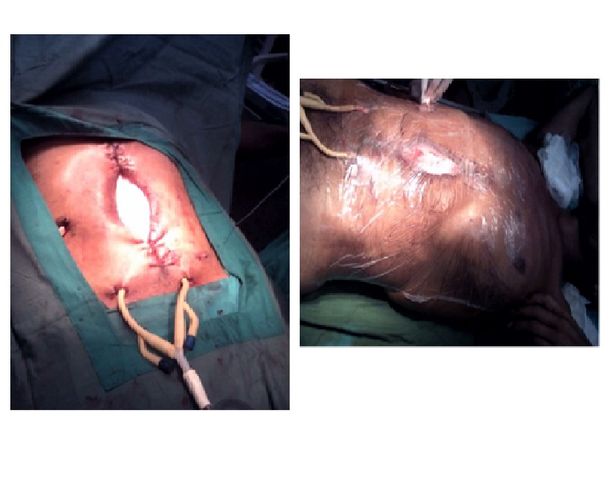
Although the intra-abdominal sepsis and anastomotic leak were controlled, the patient developed intolerance to oral intake and signs of intestinal obstruction possibly secondary to the intense visceral adhesions. Parenteral nutrition was not available at the hospital. The improvised NPWT was functional and there were multiple signs that the intraabdominal sepsis was controlled. Lab results showed normal leukocyte level levels and the patient was without fevers. Four days later, the improvised NPWT was replaced using the same procedure. The next day the patient decided to refuse further healthcare and abandoned the hospital.
DISCUSSION
High morbidity and mortality rates, 39% and 31% respectively, have been reported when gastrojejunostomy is required for malignant gastric outlet obstruction(3). This case highlights some of the early complications of a difficult foregut operation in a patient with malignancy. A high output anastomotic leak and presence of uncontrolled intra-abdominal sepsis requires emergent exploration. In a public hospital with limited resources however the challenge has just begun: managing a patient with intraabdominal sepsis and an open abdomen.
A recent systematic review describes that NPWT appears to be the most suitable temporary abdominal closure method currently available in the septic or contaminated abdomen. This method has been associated with the highest fascial closure rates. Improved outcomes were demonstrated with the use of commercial systems as opposed to vac-pack dressings using surgical towels as wound fillers(4). There are no publications regarding the use of gauze as wound filler in NPWT for temporary abdominal closure. Another important outcome to consider in these cases is incidence of new enterocutaneous or enteroatmospheric fistulas. Time to fascial or skin graft coverage of the abdomen has been shown to be related to fistula development rate. One can assume that devices, whether commercial or homemade, that control fluid output, intraabdominal sepsis and promote granulation may reduce development of fistulas. This becomes an even more important concept in resource limited settings such as this as access to parenteral nutrition as mentioned above is usually not possible.
The resource limitations in public state hospitals of developing countries considerably decrease the therapeutic alternatives in complex and complicated surgical patients. The medical uncertainty is not just what the ideal treatment of choice is, but what treatments are available at the time being. Such difficulties led to the application of an improvised emulation of NPWT. Even though a complete resolution of the patient’s morbidities was not carried out, a functional NPWT system with easily and regularly obtainable materials of low cost that successfully controlled intra-abdominal fluids and sepsis was achieved. This provided a therapeutic option that was previously unavailable in our healthcare environment. Efforts should continue to be made to develop and improve on these types of devices such that the knowledge and techniques can be brought to other limited resource settings.