John S. Young MD, Daithi S. Heffernan MD
INTRODUCTION
Necrotizing fasciitis is a rapidly spreading bacterial infection leading to necrosis of soft tissue and deep fascial involvement. Prompt surgical debridement with adjunctive supportive care are essential. Sweet’s syndrome, also known as acute febrile neutrophilic dermatosis, was first described in 1964 by Robert D. Sweet. It is characterized by the abrupt onset of tender erythematous skin lesions, diffuse infiltration of neutrophils in the dermis, prodromal symptoms or risk factors such as an underlying malignant lesion. It shows a good response to systemically administered steroids and not antibiotics. Kroshinsky first described Necrotizing Sweet’s Syndrome (NSS) in 2012. NSS is characterized by similar clinical and pathological features as necrotizing fasciitis, but in the absence of an infectious cause.
PRESENTATION
A 44 year old woman presented with a history of recurrent breast abscesses over several months. Her ED visit was prompted by an acute worsening of the pain and increase in size of the abscess prompt.
PMHx: GERD, obesity (BMI = 39)
PSHx: Excision and grafting bilateral axilla for HS
SHx: 0.5 ppd tobacco, significant socioeconomic hardship – no heat and no running water for bathing
PHYSICAL EXAM
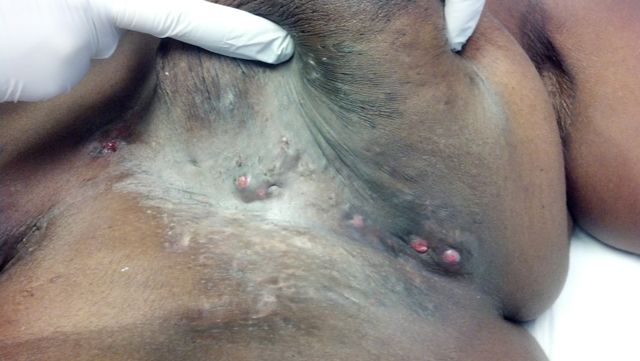
Pendulous breasts with bilateral scar tissue in the submammary and inframmary folds (IMF). Skin of the IMF was damp and macerated. The right breast had a sinus tract draining frank pus with a large area of fluctuance.
ASSESSMENT
Acute worsening of her hidradenitis given her large, pendulous breast which was only exacerbated by lack of personal hygiene with loss of access to bathing.
HOSPITAL COURSE
Incision and drainage x 2 was performed in the ED for a large amount of purulent drainage from the right breast. This was packed and the patient was admitted for wound care and further management. Meticulous wound care and personal hygiene are the mainstay of therapy. Incision and drainage when infected can be useful, however, over time inflammation and scarring result in thickened and contracted skin with nodules. While admitted the patients wounds and pain improved and she tolerated packing changes. Social work coordinated access to heated water for medical necessity.
RESULTS
The patient was discharged to home on hospital day 3 for continued wound care and hygiene particularly in the IMF and submammary region. She continued on her outpatient minocyline which she had been on chronically.
DISCUSSION
Breast involvement in HS is relatively rare though reported. Any hair bearing skin is at risk of developing HS in those with a history. Our patients course speaks to the importance of meticulous personal hygiene in the intertiginous regions to minimize risk of infection and abscess formation. Surgical management can often time include excision and grafting in severe cases. However, given the nature of our patients presentation and her large breasts we advocate for bilateral reduction mammoplasty once local wound care is achieve for ease of personal hygiene and to reduce the skin-skin redundancy seen in females with pendulous breasts.
REFERENCES
- Alharbi Z, Kauczok J, Pallua N. A review of wide surgical excision of hidradenitis suppurativa. BMC Dermatorlogy 2012; 12:9.
- Nakanishi M, Yokota K, Ochi M. Surgical Management of hidradenitis suppurtiva in the sub-mammary area. JPRAS 2010. 63, e177-e179.
- Slade DE, Powell BW, Mortimer PS. Hidradenitis suppurtiva: pathogenesis and management. Br J Plast Surg 2003; 56:451-61.
- Williams EV,et al. Combined wide excision